Histamine, DAO, Zonulin, and Mast Cells
Systems Homeostasis Perspective
This article approaches gastrointestinal, immune, and neurological reactivity through a systems homeostasis lens—focusing on regulation, tolerance, and recovery rather than symptom suppression or isolated mechanisms.
Why “Histamine Intolerance” Is Usually a Barrier and Regulation Disorder
Histamine intolerance is increasingly common in integrative and functional medicine practices. Individuals present with food reactions, flushing, headaches, anxiety, gut symptoms, rashes, palpitations, or a sense that “everything triggers me now.”
The usual explanations focus on food lists, genetics, or histamine suppression. While these approaches can reduce symptoms temporarily, they often fail to explain why tolerance was lost in the first place.
From a systems homeostasis perspective, histamine intolerance is rarely a primary histamine problem. It is most often a barrier, degradation, immune, and nervous system regulation problem.
Histamine Is a Normal Signal, Not a Toxin
Histamine is an essential signaling molecule involved in immune surveillance, gastric acid secretion, vascular tone, neurotransmission, and tissue repair.
In a regulated system, histamine rises and falls appropriately and is rapidly degraded. Problems arise not because histamine exists, but because clearance and resolution fail to keep pace with signaling load.
DAO: Degradation Capacity, Not a Cure
Diamine oxidase (DAO) is the primary enzyme responsible for degrading luminal histamine in the gut. It is produced by healthy enterocytes and functions as a first-pass clearance mechanism.
DAO capacity is reduced by intestinal inflammation, mucosal injury, oxidative stress, impaired nutrient status, and loss of epithelial integrity.
DAO supplementation can reduce symptoms, but it does not resolve the upstream reason DAO production declined. When used as a permanent strategy, it often masks barrier failure rather than correcting it. DAO is best understood as temporary load management, not resolution.
Zonulin and Barrier Regulation
Zonulin regulates intestinal tight junctions and therefore permeability. Elevated zonulin reflects loss of barrier control, allowing luminal antigens to interact with the immune system.
This has two critical consequences:
- Immune activation increases histamine release
- DAO production declines as enterocyte health deteriorates
Barrier dysfunction therefore both raises histamine signaling and reduces histamine clearance at the same time.
Mast Cells: Effectors, Not the Root Cause
Mast cells are highly sensitive immune sentinels concentrated at barrier surfaces. In a regulated system, mast cell activation is precise, proportional, and self-resolving.
In dysregulated systems, mast cells become chronically reactive—not because they are defective, but because the environment remains threatening.
Drivers of mast cell overactivity include:
- barrier disruption
- persistent immune signaling
- impaired histamine degradation
- nervous system threat signaling
Mast cells are responding appropriately. The system is failing to resolve the signal.
Nervous System Signaling and Histamine Reactivity
Mast cells express receptors for stress-related neuropeptides such as CRH and substance P. Chronic stress, sympathetic dominance, and low vagal tone lower the activation threshold for mast cell degranulation.
This explains why symptoms flare with stress, feel unpredictable, and often improve when the system is calmed—even before laboratory markers normalize.
Histamine intolerance is therefore both an immune and a neuro-regulatory phenomenon.
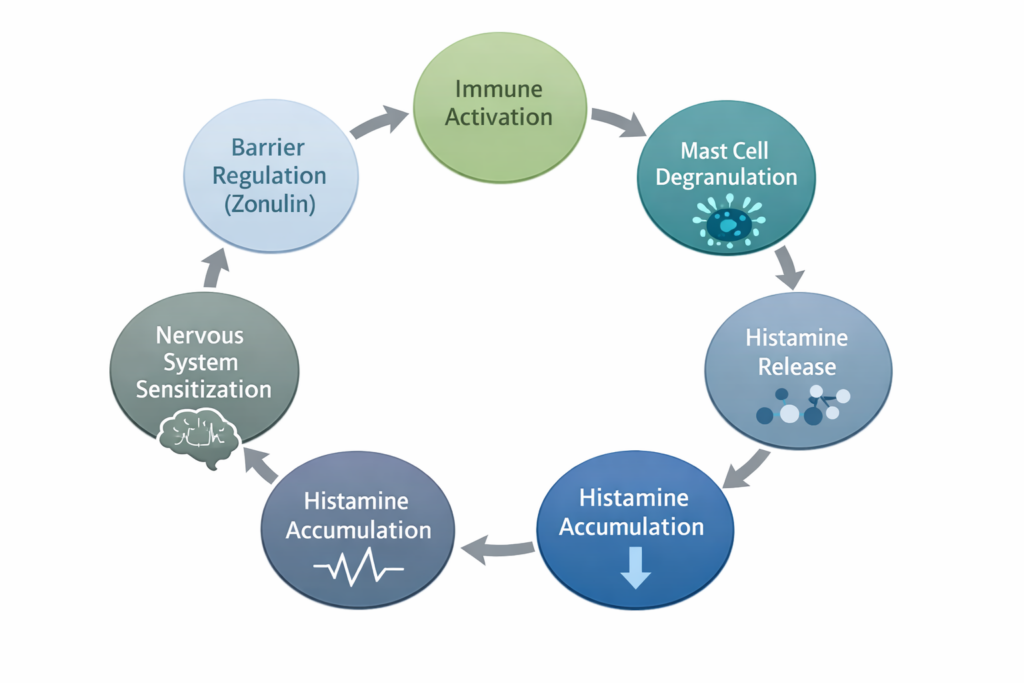
The Systems Loop
Taken together, the pattern is clear:
Barrier disruption (zonulin)
→ immune activation
→ mast cell degranulation
→ histamine release
→ reduced DAO clearance
→ histamine accumulation
→ nervous system sensitization
→ further mast cell activation and barrier stress
Suppressing one node shifts load elsewhere. Resolution requires restoring regulation.
Why Food Avoidance and DAO Alone Fail
Low-histamine diets and DAO supplementation reduce incoming load but do not restore barrier integrity, normalize immune tone, rebuild enzymatic capacity, or recalibrate nervous system signaling.
Over time, restriction often reduces resilience further, reinforcing sensitivity instead of restoring tolerance.
A note on Mast Cell Activation Syndrome (MCAS)
It’s important to distinguish between mast cell overactivity within a dysregulated system and true mast cell activation syndromes.
Many individuals experiencing histamine intolerance do not have primary mast cell disease. In these cases, mast cells are responding appropriately to unresolved immune, barrier, and nervous system threat signals.
There are, however, situations where mast cell activation becomes persistent and poorly regulated, requiring a different level of clinical consideration. Because this distinction matters—both clinically and ethically—a separate article will follow examining Mast Cell Activation Syndrome (MCAS) through a systems homeostasis lens.
Systems Reminder
Interventions only work when the system has the capacity to tolerate them.
DAO reduces histamine load.
Tolerance returns only when barrier regulation, immune signaling, and nervous system tone are restored.
How I Work
I approach health, formulation, and clinical decision-making through a systems homeostasis framework, prioritizing capacity, tolerance, recovery, and regulation before escalation. Rather than chasing symptoms, markers, or isolated pathways, I focus on sequencing interventions so the system can safely respond instead of being overwhelmed.