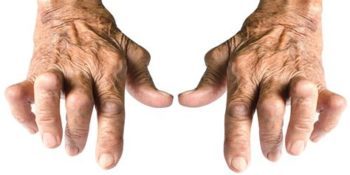
Today I wanted to share with you some published research which suggests that a common and readily accessible nutritional compound – 5-HTP may be able to mitigate the severity of Rheumatoid Arthritis (RA) and if it is consumed early on in the development stage of RA that it may in fact prevent the RA from developing.
Note that this study was done using an animal model – mice.
Rheumatoid Arthritis
From the Rheumatoid Arthritis. org website:
Rheumatoid arthritis (RA) is a complex disease that affects each patient differently. People from all ethnic backgrounds are at risk of developing RA. It is the third most common type of arthritis behind osteoarthritis and gout.
RA Facts and Statistics
RA is a chronic disease affecting over 1.3 million Americans and as much as 1% of the worldwide population. The specific cause of RA is not known, and as a result there is no known cure for the disease.
Researchers do know, however, that RA is the result of an autoimmune disorder. It is one of the most common autoimmune disorders – more common than psoriasis, Crohn’s disease, multiple sclerosis, and lupus. RA symptoms are triggered when a person’s antibodies mistakenly attack the normal synovial joint fluid, causing chronic inflammation.
Women are up to three times more likely to develop RA than men. Women are also more likely to develop the disease at a younger age than men. RA generally begins to affect people between the ages of 30 and 60 years old. The average person doesn’t develop symptoms of RA until they reach their 60’s.
————————————————————————————————-
Following is an article from the Life Enhancement website which discusses this published research on 5-HTP for RA
Here is the link to the actual abstract if you want to review it.
In the article, it suggests that 5-HTP can be useful for Asthma, Depression, Obesity, Headaches, Fibromyalgia, Insomnia, and Arthritis.
Regards,
Rob
In addition to its use as an antidepressant …
New research brings additional clarity to the mechanisms of 5-HTP
The amino acid tryptophan is essential for humans, meaning the body cannot synthesize it and must obtain it from the diet. A tryptophan deficiency can lead to serious emotional imbalances as well as diminished neural health.
In part, this is because tryptophan is a precursor to serotonin and melatonin. To synthesize these, tryptophan drives two major metabolic pathways: the serotonin pathwayand kynurenine pathway.
The Pathway to Well-Being and Happiness
In the serotonin pathway, tryptophan is catalyzed into 5-hydroxytryptophan (5-HTP) by tryptophan hydroxylase-1 and then converted into serotonin. Biochemically derived from tryptophan or 5-HTP, serotonin is principally found in the gastrointestinal tract, blood platelets, and the central nervous system of humans and animals. Serotonin is generally thought to be a contributor to feelings of well-being and happiness.
Does Kynurenine Provide a Pathway to Inflammation?
A tryptophan deficiency can lead to
serious emotional imbalances as well
as diminished neural health.
In the kynurenine pathway, tryptophan is catalyzed into N-formylkynurenine by indoleamine 2,3 dioxygenase (IDO) and then converts into L-kynurenine. L-kynurenine is a metabolite of the amino acid L-tryptophan used in the production of niacin. However, the Kynurenine pathway is a mixed bag. Rheumatoid arthritis patients have increased kynurenine levels in their blood1,2 and its levels are positively correlated with C- Reactive Protein (CRP), a measure of inflammation.3
Serotonin is generally thought to be a
contributor to feelings of well-being
and happiness.
5-HTP Suppresses Inflammatory Responses
In a new Taiwan study,4 researchers note that 5-HTP suppresses inflammatory responses in mouse models of asthma and sepsis. In prior studies, 5-HTP inhibited the production of pro-inflammatory mediators in different cell lines. These associations stimulated the researchers interest in whether 5-HTP could suppress inflammation and disease activity in collagen-induced arthritis (CIA) in mice. CIA is an animal form of human rheumatoid arthritis (RA).
The Value of Rheumatoid Arthritis’s Therapeutic Window
Evidence is accumulating that a preclinical phase is present before the onset of clinical signs and symptoms of RA. This phase represents an important therapeutic window within which interventions can dramatically modulate outcomes.
RA is a chronic inflammatory disorder that, unlike the wear-and-tear damage of osteoarthritis, typically affects the small joints in the hands and feet. RA also affects the lining of joints, causing a painful swelling that can eventually result in bone erosion and joint deformity. RA can occur at any age, although it usually begins after age 40 and is much more common in women.
Preventative Desired
An agent that could prevent RA in the preclinical phase would be a novel approach. In this study, the Taiwan researchers investigated whether the tryptophan metabolite, 5-HTP, could act as such an agent for the primary prevention of CIA. The CIA mouse model is the most commonly studied autoimmune model of rheumatoid arthritis. It is widely used to address questions of disease pathogenesis and to validate therapeutic targets.
5-HTP suppresses
inflammatory responses in mouse
models of asthma and sepsis.
5-HTP Suppressed Cell Proliferation
The Taiwan researchers found that 5-HTP given at 10, 20 and 50 μg/ml suppressed cell proliferation and decreased the production of Interleukin (IL)-22 type cells, which regulate the pathogenesis of autoimmune diseases.
5-HTP also suppressed the expression of IL-17, TNFα, IFNγ and T-bet in activated splenocytes (spleen cells). These findings did not result from cell death, because 5-HTP did not increase cell death at these levels.
It’s a Matter of Timing
In their animal studies, a supplement of 5-HTP from day 20 did not affect the disease course. However, 5-HTP given from day 7 before induction significantly decreased the arthritis scores and joint inflammation. Earlier was better than later.
5-HTP May Prevent RA
According to the Taiwan study, patients with allergy/asthma commonly have associated symptoms of anxiety/depression. These results suggest that 5-HTP supplements can be an approach to prevent arthritis.
5-HTP taken orally suppressed allergic lung inflammation, even though cytokine levels were not decreased on broncho-alveolar lavage (BAL).5 BAL is a medical procedure in which a bronchoscope is passed through the mouth or nose into the lungs and fluid is squirted into a small part of the lung and then collected for examination. It is typically performed to diagnose lung disease. (See “Galantamine Protects Against Lung Injury,” the sidebar in the lead article “Stop Smoking with Galantamine” in this issue.)
5-HTP given from day 7 before
induction significantly decreased the
arthritis scores and joint
inflammation.
Serotonin and Major Depressive Disorders
Decreased levels of serotonin in the central nervous system are associated with major depressive disorders. Treatment with selective serotonin reuptake inhibitors (SSRIs) or supplementation with serotonin precursors (tryptophan and 5-HTP) is an important strategy in depression therapy. SSRIs can block serotonin re-uptake and thus increase serotonin levels in the brain and improve depression. Tryptophan and 5-HTP can make serotonin in the body and also improve depression.
SSRIs and Supplements
Of interest, certain SSRIs can decrease the production of pro-inflammatory cytokines, suppress airway inflammation in asthma patients, and reduce disease activity in RA patients. SSRIs have also been found to decrease the arthritis scores in CIA mice and suppress cytokine production in macrophages and synovial membrane cells. But SSRIs are not without adverse effects.
Patients with allergy/asthma
commonly have associated symptoms
of anxiety/depression.
The Taiwan researchers found that the SSRI fluoxetine (aka Prozac) effectively decreased the production of IFNγ and TNFα in activated splenocytes. In the animal study, it was found that 5-HTP given orally increased the serum levels of serotonin, whereas parenteral 5-HTP did not affect the serum levels of serotonin in CIA mice. Thus, regulation of serotonin levels is not likely to be the major mechanism behind the suppression of arthritis by 5-HTP in the CIA mice.
RA patients have increased kynurenine levels in the blood, and the levels are positively correlated with C-reactive protein. In addition, RA patients have increased indoleamine 2,3 dioxygenase (IDO) activity in the synovial fluid.
5-HTP Regulates Immune Responses
The Taiwan study provides both in vitro and in vivo evidence that 5- HTP, a tryptophan metabolite, can regulate immune responses. Taking a 5-HTP supplement before CIA induction can decrease disease activity, suppress joint inflammation and cause minimal side effects in CIA mice. Nevertheless (you’ve undoubtedly heard this before), further studies are required to elucidate whether the common dietary supplement 5-HTP can act as an agent for primary prevention of RA.
5-HTP taken orally
suppressed allergic lung
inflammation, even though cytokine
levels were not decreased on
broncho-alveolar lavage.
Also in the Taiwan study, it was found that 5-HTP did not affect the cytokine levels in the serum or the percentages of IFNγ+CD4+ T cells in the spleen. However, 5-HTP suppressed the expression of TNFα and IL-6 in the inflamed ankle joints and decreased the percentages of IFNγ+CD4+ T cells in the draining lymph nodes. These results suggest that 5-HTP decreased arthritis activity without affecting systemic immunity.
Serotonin Up; Kynurenine Down
Of great interest, pro-inflammatory cytokines such as TNFα, IL-1 and IFNγ can increase IDO expression and promote serotonin re-uptake, resulting in increased levels of kynurenine and decreased levels of serotonin. Indeed, IDO is the first and rate-limiting enzyme of tryptophan catabolism through the kynurenine pathway, thus causing depletion of tryptophan, which can cause halted growth of microbes as well as T cells.
The study showed that mice with a higher arthritis score were more likely to have high serum levels of kynurenine and low levels of serotonin.
5-HTP for Asthma, Depression, Obesity, Headaches, Fibromyalgia, Insomnia, and Arthritis
As reported by the Taiwan scientists, in mouse models of asthma, the amount of 5-HTP given to the mice was equivalent to consumption of 200 mg per day by a 100 lb person. In their study, the daily consumption of 5-HTP was equivalent to between 384 mg and 1,920 mg per day by a 132 lb person.
5-HTP given orally increased the
serum levels of serotonin.
5-HTP is indicated for depression, obesity, headaches, fibromyalgia and insomnia. A 5-HTP supplement is well-tolerated and causes minimal side effects. In clinical studies, the doses of 5- HTP in the treatment of depression have been from 20 to 3,250 mg per day.
Treatment with 5- HTP at 600 mg per day was also found to decrease the frequency of migraine and improve insomnia. In a mouse model of asthma, the amount of 5-HTP given to the mice was equivalent to consumption of 200 mg per day by a 100 lb person.
In the Taiwan animal study, 5-HTP given orally did not affect body weight or cause diarrhea. However, the daily consumption of 5-HTP was equivalent to 384 mg and 1,920 mg per day by a 132 lb person. Furthermore, 5-HTP given by i.p. injection at 30, 100 and 300 mg/kg decreased the production of TNFa in a sepsis model.
These results suggest that 5-HTP
decreased arthritis activity without
affecting systemic immunity.
The mice receiving the i.p. amounts at 30, 100 and 300 mg/kg (human equivalents of 160 mg, 527 mg, 1,580 for a 132 lb person) had improved arthritis scores and decreased joint inflammation.