When discussing cardiovascular health, inflammation, or chronic disease risk, most conversations focus on cholesterol, blood pressure, or glucose. Yet one critical physiological factor is rarely discussed outside of advanced clinical and research settings: zeta potential.
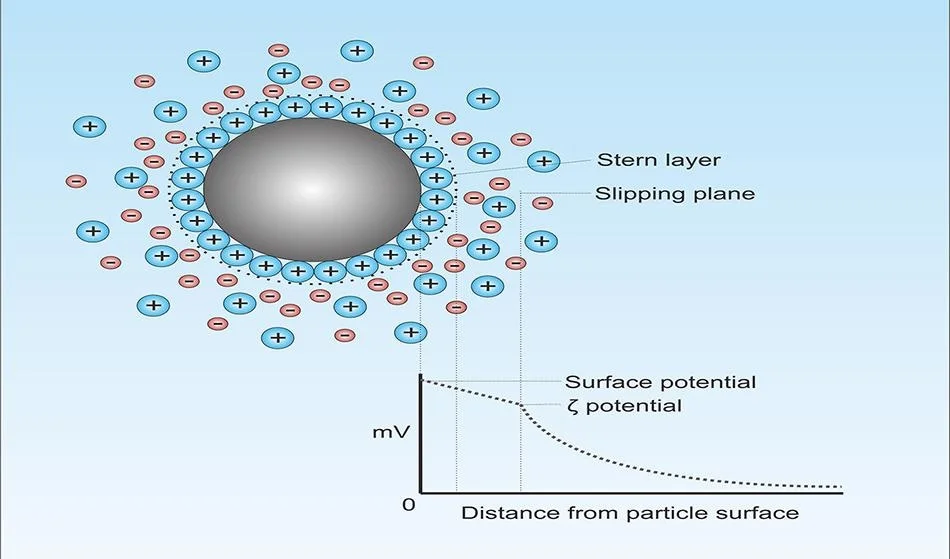
Zeta potential refers to the electrical charge on the surface of cells suspended in fluid, including red blood cells, platelets, and other circulating particles. This electrical charge determines whether cells repel each other and flow freely or clump together, impairing circulation.
What Is Zeta Potential?
Red blood cells naturally carry a negative surface charge. When this charge is strong, cells repel one another, maintaining proper spacing and allowing blood to flow smoothly through even the smallest capillaries.
When zeta potential is reduced, cells begin to aggregate (a phenomenon sometimes referred to as rouleaux formation). This increases blood viscosity, reduces microcirculation, and places greater strain on the cardiovascular system.
Why Zeta Potential Matters for Health
🔴 Acute Implications
- Sluggish blood flow
- Reduced oxygen and nutrient delivery
- Increased clotting tendency
- Impaired tissue perfusion during stress, illness, or dehydration
🔵 Chronic Implications
Persistently low zeta potential has been associated with:
- Chronic inflammation
- Cardiovascular disease risk
- Hypertension
- Metabolic dysfunction
- Autoimmune and inflammatory conditions
- Neurodegenerative processes linked to impaired cerebral circulation
Poor microcirculation can amplify metabolic chaos, where multiple physiological systems become stressed simultaneously rather than one isolated “root cause.”
What Lowers Zeta Potential?
Several common modern stressors reduce cellular charge and promote aggregation:
- Chronic dehydration
- High blood sugar and insulin resistance
- Oxidative stress
- Inflammatory cytokines
- Poor electrolyte balance
- Excess positively charged proteins and lipids
- Chronic sympathetic (stress) dominance
Supporting Healthy Zeta Potential
Strategies that support cellular charge and blood flow include:
- Adequate hydration with proper electrolytes
- Supporting antioxidant status
- Reducing inflammatory burden
- Improving metabolic flexibility
- Supporting liver and gut function (which influence plasma proteins)
- Optimizing mineral balance
This systems-based approach improves flow, oxygen delivery, and cellular resilience rather than targeting isolated symptoms.
Why This Matters Clinically
Zeta potential provides insight into how well blood can actually deliver oxygen and nutrients, not just what appears on standard labs. It helps explain why some individuals experience fatigue, cold extremities, brain fog, or exercise intolerance despite “normal” conventional markers.
🔹 Work With Me
Formulation & Product Development
If your company or clinic is developing nutritional supplements or functional drinks, I provide consulting and formulation services to help create science-driven, evidence-based products that support circulation, metabolic resilience, and systemic health.
Clinical Support
If you’re struggling with ongoing symptoms and feel you’ve been told “everything looks normal,” I work with individuals using lab-informed, systems-based support to address metabolic chaos and restore physiological resilience.
👉 Learn more: OptimumHealthConsulting.com
#ZetaPotential #Microcirculation #MetabolicHealth #Inflammation #Healthspan #FunctionalNutrition #RobLamberton #RobertLamberton


 Compounding formulation (sterile & non-sterile)
Compounding formulation (sterile & non-sterile) Development of a 46-SKU botanical precision-medicine range
Development of a 46-SKU botanical precision-medicine range Operational systems & quality assurance integration
Operational systems & quality assurance integration Practitioner education programs in functional nutrition, integrative medicine, and metabolic assessment
Practitioner education programs in functional nutrition, integrative medicine, and metabolic assessment Clinical translation of regenerative and longevity protocols
Clinical translation of regenerative and longevity protocols